Bariatric Surgery has emerged as one of the most researched and transformative interventions for individuals struggling with severe obesity and related metabolic disorders. Beyond aesthetic change, Bariatric Surgery represents a complex metabolic intervention that influences hormones, appetite regulation, insulin sensitivity, and systemic inflammation. At WellDemir, we approach this topic not as a trend, but as a scientifically grounded pathway that continues to evolve through clinical research and patient centered innovation.
Long term weight management is rarely about willpower alone. Obesity is increasingly understood as a chronic, relapsing metabolic condition shaped by genetics, neurohormonal signals, gut microbiota, and environmental factors. Within this framework, Bariatric Surgery functions as more than a restrictive tool. It reshapes physiological pathways that influence how the body stores and utilizes energy.
The Science Behind Bariatric Surgery and Metabolic Regulation
Bariatric Surgery procedures, including gastric bypass and sleeve gastrectomy, influence metabolic pathways in ways that extend beyond simple calorie reduction. Clinical observations suggest that hormonal changes following metabolic surgery occur rapidly, sometimes even before significant weight loss is achieved.
Get Free Consultation
Have any questions? Leave your details and we'll get back to you shortly.
After surgical intervention, levels of gut hormones such as GLP 1 and peptide YY may increase. These hormones are associated with satiety and improved insulin response. Simultaneously, ghrelin levels, often referred to as the hunger hormone, may decrease depending on the procedure. This hormonal recalibration helps explain why Bariatric Surgery is often associated with improved blood sugar control and metabolic balance.
Emerging research published in leading metabolic journals indicates that insulin sensitivity may improve within weeks. While individual outcomes vary, the metabolic shift appears to involve a coordinated interaction between the gastrointestinal tract and endocrine system.
How Bariatric Surgery Contributes to Sustainable Weight Loss
Weight loss achieved through Bariatric Surgery differs from conventional dieting in its durability and physiological basis. Diet induced weight loss often triggers compensatory mechanisms such as increased hunger and reduced metabolic rate. Surgical weight loss, however, appears to modify some of these adaptive responses.
Several longitudinal studies tracking patients for 10 to 15 years have reported sustained weight reduction in many individuals undergoing metabolic surgery. The combination of reduced stomach capacity, altered nutrient absorption in some procedures, and neurohormonal adaptation may contribute to long term results.
It is important to note that sustainability is influenced by behavioral adaptation, nutritional monitoring, and psychological readiness. Bariatric Surgery may provide a metabolic advantage, but lifestyle integration remains an essential factor in long term outcomes.
Types of Bariatric Surgery and Their Mechanisms
Different forms of Bariatric Surgery operate through distinct physiological mechanisms. Below is a simplified comparison:
| Procedure | Primary Mechanism | Metabolic Impact |
| Gastric Sleeve | Stomach volume reduction | Hormonal modulation and appetite suppression |
| Gastric Bypass | Restriction and mild malabsorption | Enhanced insulin sensitivity and gut hormone shifts |
| Mini Gastric Bypass | Simplified bypass pathway | Altered nutrient flow and metabolic recalibration |
Each technique may influence glucose metabolism, lipid profiles, and inflammatory markers differently. The choice of procedure is typically individualized, taking into account medical history, metabolic profile, and clinical assessment.
While all forms of metabolic surgery aim to reduce excess weight, their endocrine effects are a major focus of current scientific exploration.
Bariatric Surgery and Type 2 Diabetes Remission
One of the most widely discussed aspects of Bariatric Surgery is its relationship with type 2 diabetes improvement. Several multicenter trials have reported significant reductions in HbA1c levels following metabolic procedures.
Interestingly, improvements in blood glucose control often occur before substantial weight reduction. This phenomenon has led researchers to investigate the role of altered bile acid circulation, incretin hormones, and gut microbiome changes.
Although remission rates vary, the metabolic improvements associated with Bariatric Surgery have shifted global guidelines. Organizations such as the World Health Organization and the American Diabetes Association acknowledge metabolic surgery as a consideration for certain patients with obesity related diabetes.
These endorsements reflect the growing recognition of obesity as a metabolic disease rather than solely a lifestyle condition.
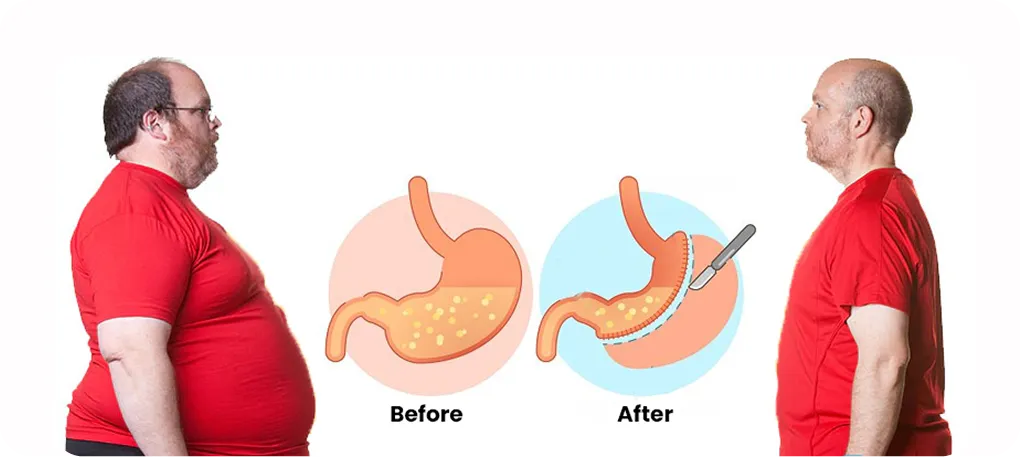
Long Term Cardiovascular and Inflammatory Benefits of Bariatric Surgery
Beyond glucose control, Bariatric Surgery may influence cardiovascular risk factors. Studies tracking lipid profiles have observed reductions in triglyceride levels and increases in HDL cholesterol in many patients.
Chronic inflammation, often elevated in obesity, may also decline after surgical weight loss. Markers such as C reactive protein have shown downward trends in observational cohorts. While causality is complex, the data suggest that metabolic surgery may contribute to systemic improvements beyond weight alone.
Researchers are also examining how Bariatric Surgery affects endothelial function, arterial stiffness, and long term cardiac events. Although ongoing studies continue to refine our understanding, early evidence indicates potential cardiometabolic advantages.
Psychological and Behavioral Dimensions After Bariatric Surgery
The metabolic transformation initiated by Bariatric Surgery is intertwined with psychological adaptation. Rapid weight change can alter body image perception, social interactions, and self identity.
Behavioral research suggests that structured follow up programs enhance long term success. Nutritional counseling, peer support, and mental health evaluation may help individuals adapt to new eating patterns and lifestyle rhythms.
Interestingly, some patients report changes in taste preferences and reward sensitivity after metabolic surgery. These shifts may reflect neurological and hormonal changes that influence food related decision making.
In this context, Bariatric Surgery is not merely a physical intervention. It intersects with neurobiology, psychology, and social dynamics in a multidimensional way.
Risks, Considerations, and Evidence Based Evaluation
Like all surgical interventions, Bariatric Surgery carries potential risks. These may include nutritional deficiencies, surgical complications, or the need for revision procedures. Modern techniques and standardized protocols have contributed to improved safety profiles compared to earlier decades.
Data from international registries suggest that complication rates are comparable to other commonly performed abdominal surgeries. Nevertheless, candidacy assessment is essential. Multidisciplinary evaluation typically includes metabolic screening, psychological assessment, and nutritional planning.
Understanding the full scope of Bariatric Surgery requires balancing potential benefits with realistic expectations. Evidence based medicine emphasizes informed decision making rather than oversimplified narratives.
The Future of Bariatric Surgery and Metabolic Innovation
Research into Bariatric Surgery continues to expand into new territories. Scientists are investigating how gut microbiota diversity shifts after surgery and how these changes influence metabolism. Some studies suggest that microbial composition may partially mediate insulin sensitivity improvements.
There is also growing interest in less invasive endoscopic techniques and personalized metabolic profiling. The integration of genomics and artificial intelligence into metabolic research may further refine patient selection and outcome prediction.
At WellDemir, our perspective on Bariatric Surgery is grounded in continuous education, multidisciplinary collaboration, and respect for scientific progress. The field no longer revolves solely around weight reduction. It is increasingly recognized as a branch of metabolic medicine.
Bariatric Surgery represents a significant development in the understanding and management of obesity and metabolic disorders. By influencing hormonal pathways, insulin dynamics, inflammation, and appetite regulation, it offers a multifaceted approach to long term weight loss.
Rather than framing metabolic surgery as a shortcut, contemporary research positions it as a scientifically validated tool within a broader health strategy. Outcomes vary, and individual assessment remains central. Yet the growing body of global evidence continues to highlight the metabolic depth of Bariatric Surgery.
For individuals exploring advanced options for sustainable weight management, understanding the science behind Bariatric Surgery provides clarity beyond headlines. At WellDemir, we believe informed knowledge empowers confident decisions.



