Gum Pain can turn ordinary moments into surprisingly difficult ones. A sip of cold water, a crunchy snack, or even a casual smile may suddenly feel uncomfortable. While many people think of sore gums as a small and temporary issue, gum pain can sometimes reflect irritation, inflammation, pressure, injury, or underlying oral changes that deserve closer attention.
At WellDemir, we believe good health content should be clear, grounded in science, and easy to read. That is especially true for a topic like gum pain, because the causes can range from something simple, such as brushing too hard, to more complex factors involving plaque, oral bacteria, hormonal changes, ulcers, or gum disease. Understanding what may be happening inside the mouth helps readers make sense of the discomfort without panic, guesswork, or misinformation.
Table of Contents
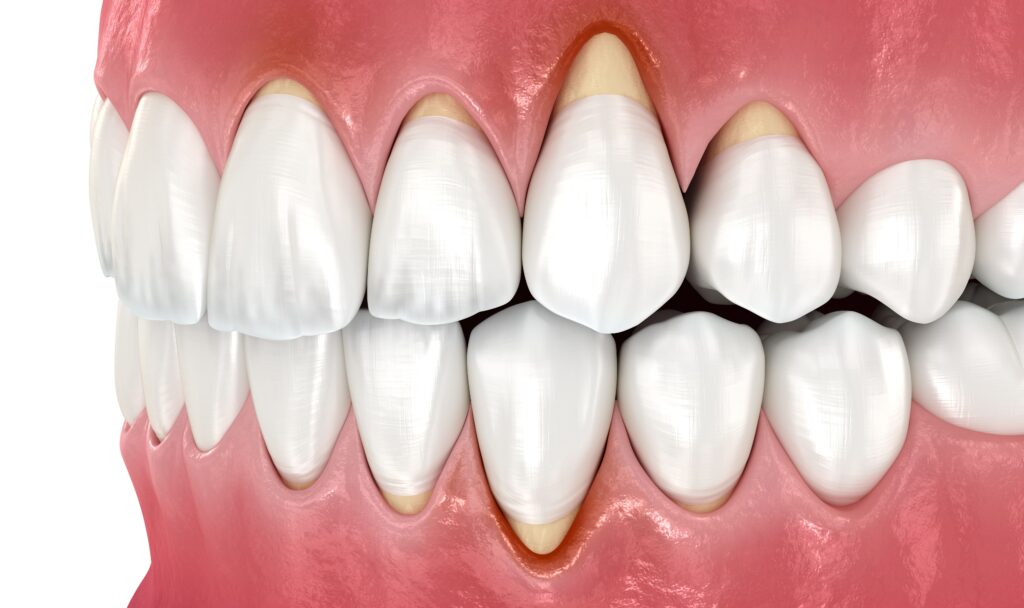
Understanding Gum Pain and Why It Happens
Gum pain is not a single condition. It is a symptom, and symptoms often have many possible explanations. Gum tissue is delicate, highly vascular, and constantly exposed to food particles, temperature changes, bacteria, and friction. Because of that, even mild irritation can be noticeable.
Get Free Consultation
Have any questions? Leave your details and we'll get back to you shortly.
In many cases, discomfort begins when the gum tissue becomes inflamed. Inflammation is the body’s response to irritation or injury. If plaque accumulates near the gumline, the immune system may react to bacterial activity. This can lead to swelling, redness, tenderness, and a sore or throbbing sensation. For some people, gum pain feels localized to one area. For others, it may feel diffuse and affect several parts of the mouth.
There is also a mechanical side to sore gums. A hard-bristled toothbrush, aggressive flossing, poorly fitting dental appliances, or sharp foods can place pressure on the tissue. The result may be a painful spot, especially if the gum surface is already sensitive. This is why the same symptom, gum pain, can have dramatically different causes depending on the context.
Researchers and oral health organizations often describe gum discomfort as a signal rather than a disease itself. According to information from the National Institute of Dental and Craniofacial Research, gum symptoms often overlap with broader oral health patterns, especially when inflammation is involved. That is one reason persistent soreness tends to attract clinical interest.
Common Causes of Gum Pain in Daily Life
One of the most common causes of gum pain is plaque buildup. Plaque is a sticky biofilm made of bacteria, saliva, and food debris. If it is not removed regularly, it may irritate the gums and contribute to gingival inflammation. This is often one of the earliest and most frequent explanations for mild to moderate discomfort.
Another everyday cause is brushing technique. Many people assume that brushing harder means cleaning better. In reality, excessive force can wear down soft tissue and create tenderness. Flossing too aggressively can also make the gums sore, particularly if someone is new to flossing or resumes the habit after a long break.
Hormonal shifts may also influence gum pain. Some individuals notice more sensitivity during pregnancy, menstruation, or menopause. These changes may affect how the gum tissue responds to plaque and irritation. In such cases, the gums can seem more reactive than usual, even when oral hygiene routines have not changed much.
Diet can contribute too. Very hot foods, sharp chips, acidic fruit, and sugary snacks may irritate vulnerable gum tissue. Tobacco use, dry mouth, and stress-related habits such as clenching can further complicate the picture. None of these factors guarantees gum pain, but they can increase the chances of discomfort in a susceptible mouth.
Below is a quick overview of common contributing factors:
| Possible Factor | How It May Affect the Gums |
|---|---|
| Plaque buildup | May trigger inflammation and tenderness |
| Hard brushing | Can irritate or injure gum tissue |
| Aggressive flossing | May cause localized soreness or bleeding |
| Hormonal changes | May increase gum sensitivity |
| Mouth ulcers | Can create painful spots near the gums |
| Dry mouth | May reduce natural protection in the mouth |
| Tobacco use | May irritate tissue and affect healing |
| Poorly fitting dental devices | May create friction and pressure |
Signs That Gum Pain May Be Linked to Inflammation
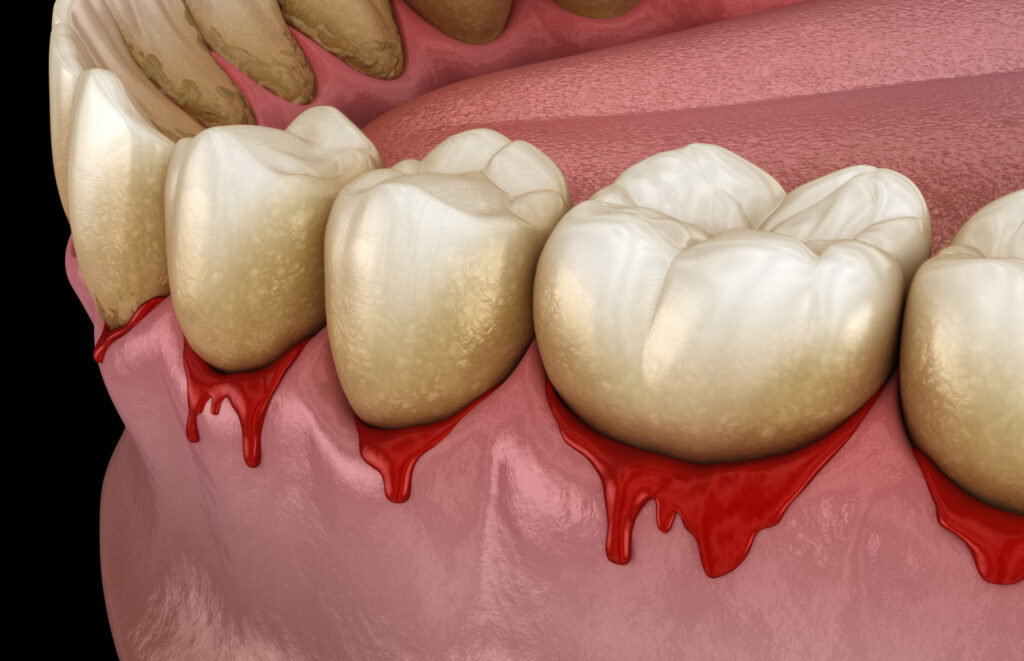
Not all gum pain looks the same. Sometimes the gums appear redder than usual. Sometimes they look puffy or bleed during brushing. In other cases, the tissue may feel tender but appear almost normal. The way inflammation presents can vary widely from person to person.
One pattern often associated with inflammatory gum issues is discomfort near the gumline, especially if there is visible plaque or tartar. A person may notice bad breath, mild swelling, or bleeding with brushing. These signs can point toward gingivitis, a common early-stage gum condition related to plaque accumulation. Gingivitis does not always cause severe pain, but when the tissue becomes irritated enough, gum pain can definitely occur.
If the discomfort seems to come and go, that may suggest fluctuating irritation. For example, a person may feel better after cleaning the area more carefully, then worse again after eating certain foods or missing oral hygiene for a few days. This up-and-down pattern often reflects local inflammation rather than sudden injury alone.
There are also cases in which sore gums are connected to more advanced periodontal changes. In those situations, symptoms might include gum recession, deeper tenderness, or discomfort when chewing. The World Health Organization has highlighted the broad global burden of oral diseases, including gum-related conditions, emphasizing how common these issues are across populations. That wider context matters because gum pain is not unusual, even if its cause is not always obvious at first.
Gum Pain Around One Tooth Versus All Over the Mouth
Location matters. Gum pain around one tooth may suggest a very different issue than soreness spread across the entire mouth. A single painful area might be related to trapped food, a sharp tooth edge, a canker sore, local trauma, or pressure from a nearby tooth. Sometimes even a popcorn hull can create intense discomfort if it becomes wedged near the gumline.
On the other hand, widespread tenderness may point toward generalized inflammation, oral irritation, or a systemic factor affecting the tissues more broadly. If many areas feel sore at once, possibilities may include gingival inflammation, hormonal sensitivity, viral irritation, dry mouth, or a reaction to oral care products. Some toothpastes and mouth rinses contain ingredients that sensitive individuals may find irritating.
The texture of the discomfort can also provide clues. Sharp and sudden gum pain may be more consistent with a local irritant or injury. Dull, throbbing, or persistent tenderness may suggest inflammation or pressure. Burning sensations can sometimes be associated with chemical irritation, ulcers, or broader oral sensitivity patterns.
This distinction is useful because people often describe all oral soreness in the same way. Yet gum tissue, teeth, nerves, and oral mucosa can all produce overlapping sensations. A thoughtful description of where the pain is, when it started, and what makes it worse may reveal more than the intensity alone.
Triggers That Can Make Gum Pain Feel Worse
Certain triggers can amplify gum pain, even when the underlying cause remains the same. Temperature is a common one. Cold drinks, hot coffee, or icy desserts may increase awareness of gum sensitivity, especially if the tissue is inflamed or if gum recession exposes more vulnerable areas near the roots.
Texture matters as well. Crunchy foods, seeds, crusty bread, and spicy meals may aggravate sore gums simply by creating friction or chemical stimulation. If there is already a small ulcer or inflamed patch, these triggers can make the discomfort feel sharper and more immediate.
Stress is another often overlooked factor. Stress does not directly create all forms of gum pain, but it can influence habits that affect the mouth. People under stress may clench their jaw, neglect oral care routines, breathe through the mouth more often, or experience immune changes that alter inflammatory responses. The result may be more tenderness or a longer-lasting sense of irritation.
A few common aggravating triggers include:
- Very hot or very cold foods
- Crunchy or sharp-edged snacks
- Spicy or acidic meals
- Hard brushing or repeated rubbing
- Smoking or vaping
- Dry mouth during sleep
- Clenching or grinding habits
These triggers do not always cause the problem, but they can make existing gum pain more noticeable.
What Relief From Gum Pain Usually Depends On
Relief from gum pain often depends on the reason behind it. That may sound obvious, but it is the key point. Discomfort caused by a temporary food injury may settle differently than pain related to inflammation, mouth ulcers, or pressure around a tooth. In that sense, relief is less about finding one universal trick and more about understanding the nature of the irritation.
In general discussions of oral discomfort, gentle care is usually more helpful than aggressive self-treatment. Many people instinctively brush the sore area harder because it feels “unclean,” but that can sometimes increase irritation. A softer approach to oral hygiene may reduce friction while keeping the mouth clean. Likewise, avoiding known irritants such as very spicy or crunchy foods may make the gums feel calmer while the tissue recovers.
Hydration may matter too, because saliva plays a major protective role in the mouth. A dry environment can make sore tissues feel even more uncomfortable. If gum pain is linked to dryness, friction, or sensitivity, then a well-hydrated mouth may simply feel less irritated during the day. This is not a cure, but it helps explain why symptoms sometimes feel worse after long periods of mouth breathing or low fluid intake.
The most important idea is that relief is often contextual. If the discomfort is brief and clearly related to a minor trigger, it may resolve as the tissue settles. If gum pain keeps returning, spreads, or comes with swelling, bleeding, or persistent tenderness, the underlying explanation may need closer attention.
When Gum Pain May Deserve Closer Attention
A short episode of gum pain may happen to almost anyone. The mouth is a busy environment, and the gums are sensitive. But there are situations in which the pattern of discomfort may seem more significant. For example, if soreness lasts longer than expected, worsens over time, or appears alongside bleeding, bad breath, swelling, gum recession, or loose-feeling teeth, those changes may suggest something more than simple irritation.
Pain that interferes with chewing, speaking, or sleeping can also feel more concerning. Likewise, if one area remains repeatedly tender, that may indicate a local problem that is not resolving on its own. A sore spot near a crown, retainer, or wisdom tooth area may behave differently from diffuse inflammation across the front gums.
It is also worth noting that gum pain does not always stay in the gums. People sometimes describe pain in the gum when the actual source may involve the tooth, surrounding ligament, sinus pressure, or a lesion nearby. Because the mouth contains many structures in close quarters, perceived location can be misleading. That is one reason oral discomfort can feel tricky to interpret without context.
Rather than treating every sore gum episode as alarming, it makes more sense to look at the full picture. Duration, visible changes, recurrence, and associated symptoms usually tell a more useful story than pain alone.
The Science Behind Sore Gums, Healing, and Oral Sensitivity
From a biological perspective, gum pain often reflects the interaction between tissue injury, inflammatory molecules, nerve endings, and the oral microbiome. The gums are rich in blood vessels and immune activity, which is helpful for defense but also means inflammation can become noticeable quickly. When bacteria accumulate or tissue is physically irritated, the body may release signaling chemicals that increase sensitivity.
This process is not necessarily harmful in itself. Pain is often part of the body’s protective communication system. It draws attention to an area that may need rest, cleaning, or evaluation. In the mouth, however, healing can be complicated because the tissues are constantly exposed to moisture, food, movement, and microbes. That makes the experience of gum pain uniquely dynamic compared with discomfort on skin elsewhere in the body.
Another interesting point is that oral sensitivity varies widely. Two people may have similar gum inflammation but describe very different levels of soreness. Genetics, stress, immune response, pain perception, and tissue thickness may all play a role. That variability is one reason broad, one-size-fits-all explanations rarely do the topic justice.
Scientific understanding of gum discomfort continues to evolve, especially in areas involving inflammation, biofilms, and host response. The deeper researchers look, the clearer it becomes that gum pain is not a trivial complaint. It is a meaningful symptom with biological, behavioral, and environmental dimensions.
Gum pain is common, but it is not simple. It may be linked to plaque, irritation, injury, hormonal changes, ulcers, dryness, friction, or deeper gum concerns. Sometimes it appears suddenly after a clear trigger. Sometimes it develops gradually and reflects inflammation that has been building quietly over time.
The most useful way to think about gum pain is as a message, not a mystery and not a verdict. Its meaning depends on location, duration, visible changes, triggers, and the broader condition of the mouth. By understanding these patterns, readers can make better sense of what sore gums may indicate without jumping to conclusions.
At WellDemir, we aim to present health topics with clarity, balance, and substance. In the case of gum pain, that means looking beyond the symptom itself and exploring the anatomy, biology, and everyday habits that may shape it. A sore gum may be brief and minor, or it may reflect a larger oral health pattern. Either way, informed awareness is always more useful than guesswork.



