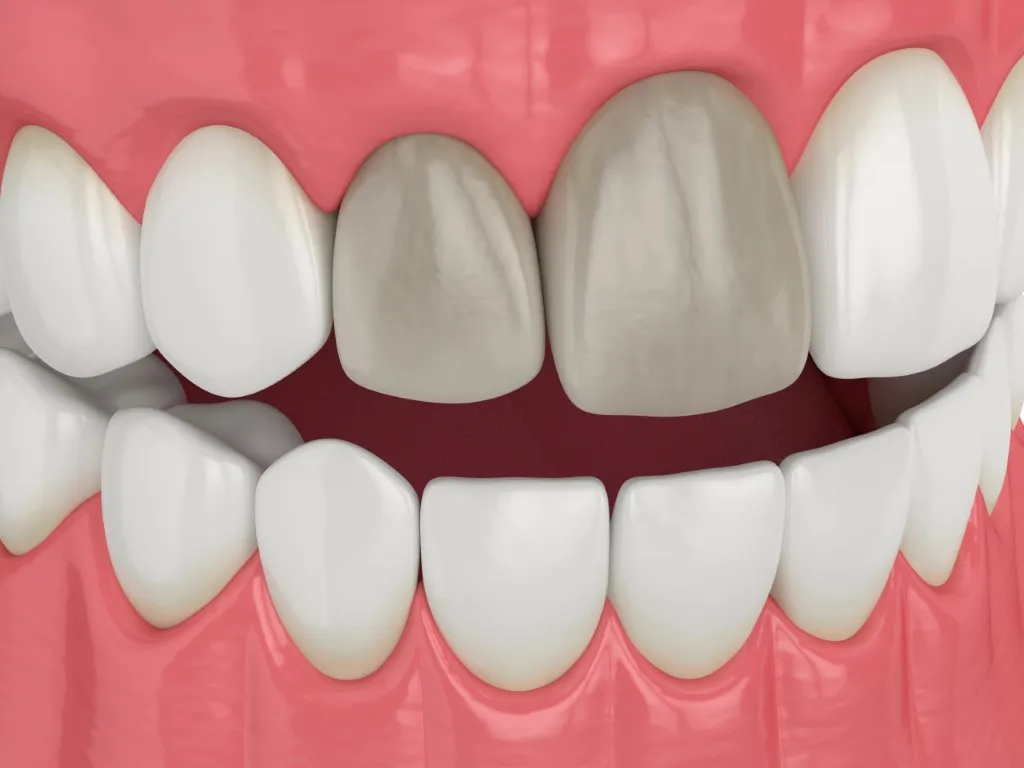
A Dead Tooth is a dental condition that often develops silently, yet its effects can be both visible and uncomfortable over time. While many people associate tooth problems with pain, a Dead Tooth may not always hurt, making it harder to detect in its early stages. Understanding what happens inside a tooth, why it “dies,” and how it can potentially be preserved is essential for anyone interested in long-term oral health.
Table of Contents
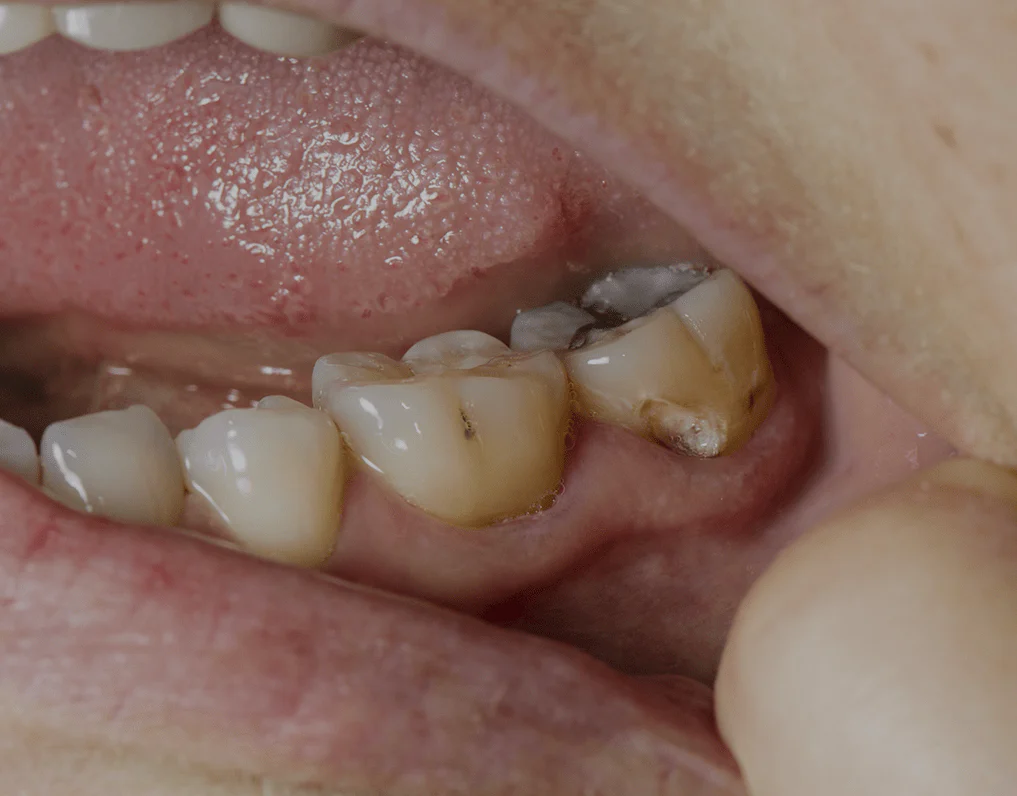
What Is a Dead Tooth and How Does It Develop?
A Dead Tooth refers to a tooth that no longer receives blood supply. Inside every healthy tooth lies a soft tissue called pulp, which contains nerves and blood vessels. When this pulp becomes damaged or infected, the tooth gradually loses vitality.
This process does not happen overnight. A Dead Tooth often evolves through stages, beginning with inflammation and progressing to complete pulp necrosis. The transformation can be subtle at first, which is why many individuals remain unaware of the issue until visible changes appear.
Get Free Consultation
Have any questions? Leave your details and we'll get back to you shortly.
Interestingly, research in dental pathology suggests that reduced blood flow within the pulp can begin long before noticeable symptoms occur. This means a Dead Tooth might exist for weeks or even months before being identified.
Common Causes of Dead Tooth Formation
Several underlying factors can lead to the development of a Dead Tooth, each affecting the internal structure of the tooth in different ways.
One of the most common causes is trauma. A sudden impact, such as a fall or sports injury, can damage the blood vessels inside the tooth. Even if the outer enamel appears intact, the internal tissue may already be compromised, eventually leading to a Dead Tooth.
Another frequent cause is untreated tooth decay. When bacteria penetrate deep into the tooth, they can infect the pulp and disrupt its function. Over time, this infection may cause the tissue to die, resulting in a Dead Tooth.
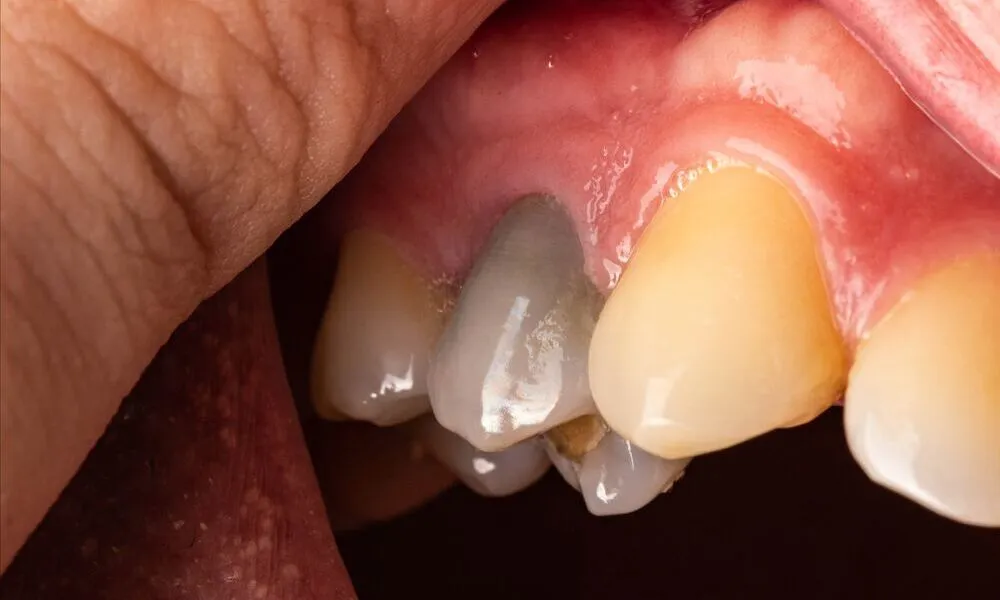
Other contributing factors include repeated dental procedures, cracks in the tooth, and prolonged pressure from grinding or clenching. Each of these conditions can interfere with the tooth’s internal health, increasing the likelihood of a Dead Tooth forming.
Symptoms That May Indicate a Dead Tooth
Recognizing the signs of a Dead Tooth can be challenging because symptoms vary widely between individuals.
One of the most noticeable indicators is discoloration. A Dead Tooth often turns yellow, gray, or even black due to changes in the internal tissue. This color shift is typically gradual but becomes more pronounced over time.
Pain is another possible symptom, although not always present. Some people experience sharp or throbbing discomfort, especially if an infection is involved. Others may feel no pain at all, which can delay diagnosis of a Dead Tooth.
Additional signs may include swelling around the gums, a persistent bad taste, or sensitivity when biting. These symptoms often suggest that the issue extends beyond the tooth itself, potentially involving surrounding tissues.
Can a Dead Tooth Be Saved?
The idea of saving a Dead Tooth may seem unlikely, but in many cases, dental interventions can preserve the structure of the tooth even after the pulp has died.
One commonly discussed approach is root canal therapy. This procedure involves removing the damaged pulp, cleaning the inner chamber, and sealing the tooth. Although the tooth is no longer “alive,” it can still function effectively within the mouth.
Another option may involve restorative treatments such as crowns. After stabilizing a Dead Tooth, a crown can help protect it from further damage while restoring its appearance.
It is important to note that outcomes vary depending on the severity of the condition. Early detection often increases the chances of managing a Dead Tooth successfully, while delayed treatment may limit available options.
Scientific Insights Into Tooth Vitality and Recovery
Modern dental research provides valuable insights into how a Dead Tooth develops and how it might be managed.
Studies in endodontics highlight the role of bacterial infection as a primary driver of pulp necrosis. Once bacteria reach the inner layers of the tooth, they trigger an immune response that can ultimately destroy the pulp tissue, leading to a Dead Tooth.
Emerging technologies also explore regenerative approaches, such as tissue engineering and stem cell therapies. While still under investigation, these methods aim to restore vitality to compromised teeth rather than simply preserving their structure.
The following table summarizes key differences between a healthy tooth and a Dead Tooth:
| Feature | Healthy Tooth | Dead Tooth |
|---|---|---|
| Blood Supply | Active | Absent |
| Color | White or natural shade | Yellow, gray, or black |
| Sensitivity | Normal | Reduced or absent |
| Internal Tissue | Vital pulp | Necrotic pulp |
Prevention Strategies to Avoid a Dead Tooth
Preventing a Dead Tooth often involves maintaining consistent oral hygiene and being mindful of potential risks.
Daily brushing and flossing play a crucial role in reducing bacterial buildup. By limiting the progression of decay, these habits can help protect the inner structures of the tooth from damage that might lead to a Dead Tooth.
Protective measures are equally important. For example, wearing a mouthguard during sports can reduce the risk of trauma, which is a leading cause of a Dead Tooth. Similarly, addressing habits like teeth grinding may help prevent long-term damage.
Regular dental check-ups also contribute to early detection. Even when symptoms are not obvious, routine examinations can reveal underlying issues before they develop into a Dead Tooth.
Long-Term Outlook for a Dead Tooth
The long-term outlook for a Dead Tooth depends on several factors, including how early the condition is identified and the type of intervention used.
In many cases, a treated Dead Tooth can remain functional for years. Advances in dental materials and techniques have improved the durability of restorative solutions, allowing individuals to maintain both function and aesthetics.
However, untreated cases may lead to complications such as infection or tooth loss. This highlights the importance of awareness and timely evaluation when signs of a Dead Tooth appear.
From a broader perspective, understanding the lifecycle of a Dead Tooth offers valuable insight into overall dental health. It emphasizes the interconnected nature of oral structures and the importance of proactive care.
A Dead Tooth is more than just a dental issue; it is a complex condition that reflects the delicate balance within the oral environment. From its gradual development to the range of possible outcomes, each stage provides insight into how teeth function and respond to damage.
By exploring the causes, recognizing the symptoms, and understanding potential management strategies, individuals can gain a clearer perspective on how to approach a Dead Tooth. While not every case can be reversed, knowledge remains a powerful tool in preserving oral health.
WellDemir continues to emphasize informed awareness and scientifically grounded information, helping readers navigate topics like the Dead Tooth with clarity and confidence.