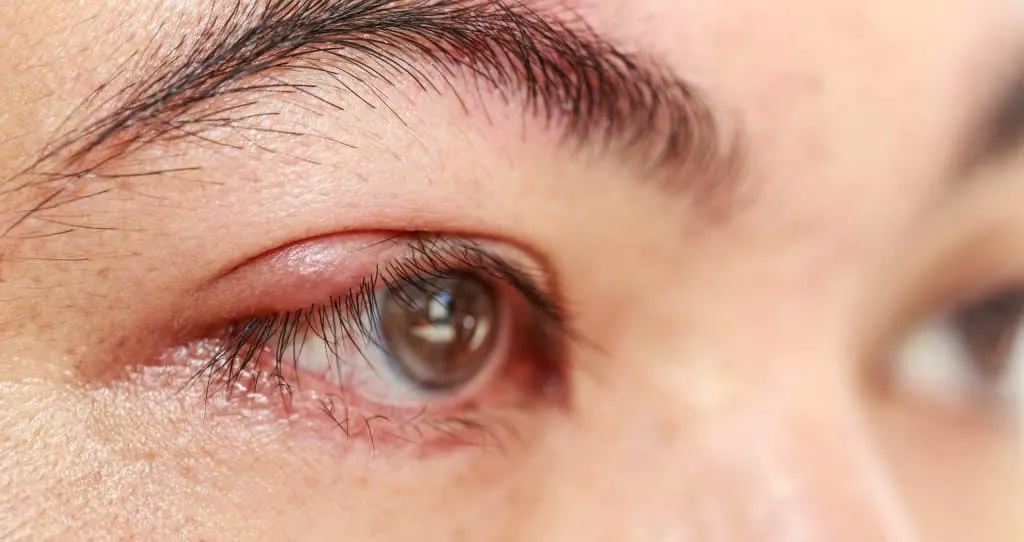
An unexpected bump on the eyelid can be more than just a minor annoyance; it is often the primary sign of stye disease. Characterized by a painful, red lump that resembles a pimple, a stye is a common bacterial eye infection that affects people of all ages. While most styes resolve with basic care, their presence often signals an imbalance in ocular hygiene or an underlying health issue that requires professional attention.
Understanding the nuances of eye diseases stye development is essential for preventing the progression of the infection. Whether you are dealing with a one-time occurrence or chronic episodes, our goal is to provide a clear, insured pathway to recovery, ensuring that your vision and comfort remain uncompromised.
Table of Contents
What is a Stye? Understanding the Basics
A stye, or hordeolum, is a localized infection of the sebaceous glands or hair follicles of the eyelid. To understand stye disease of eye anatomy, we must categorize them into two distinct types: External vs Internal stye.
Get Free Consultation
Have any questions? Leave your details and we'll get back to you shortly.
An external stye starts at the base of the eyelash, usually due to an infection in the follicle. It looks like a small, yellow-centered pimple on the edge of the lid. Conversely, an internal stye occurs in the Meibomian glands, which are responsible for producing the oil that keeps your tears from evaporating. Because internal styes are deeper within the eyelid, they often cause more significant eyelid swelling and redness and can be more painful than their external counterparts.
While a stye is primarily an acute infection, it is frequently confused with other eye diseases stye variants. The primary culprit behind this infection is the Staphylococcus bacterium, which naturally lives on the skin but can cause problems when it becomes trapped inside a gland. Proper identification is the first step in ensuring the infection does not spread to the rest of the eyelid or the ocular surface.
Why Do Styes Form? Common Risk Factors

Styes do not appear without a trigger. Usually, they are the result of a blockage in an oil gland, which creates a stagnant environment where bacteria can flourish. However, certain lifestyle factors and underlying health conditions can increase your vulnerability to stye eye disease.
- Poor Hygiene: Touching your eyes with unwashed hands or failing to disinfect contact lenses is a leading cause.
- Cosmetic Use: Using expired makeup or failing to remove eye cosmetics before sleep can clog the delicate eyelid glands.
- Underlying Skin Conditions: Conditions like rosacea or seborrheic dermatitis often lead to blepharitis, which significantly increases the risk of styes.
- Systemic and Autoimmune Factors: Some studies suggest a link between autoimmune disease and styes, where the body’s inflammatory response is heightened. Additionally, conditions like crohn’s disease eye stye correlations or graves eye disease stye complications show that systemic health and ocular health are deeply interconnected.
- Chronic Dryness: There is a strong relationship between dry eye disease and styes. When the eyes are chronically dry, the Meibomian glands often malfunction, leading to the blockages that cause internal styes.
Stye vs. Chalazion: How to Know the Difference
One of the most frequent questions patients ask is: How to tell the difference between a stye and a chalazion? While they both appear as lumps on the eyelid, their causes and treatments are quite different.
Stye (Hordeolum):
- Pain: Usually very painful and tender to the touch.
- Appearance: Red, swollen, and often has a visible “head” or pus point.
- Cause: An acute bacterial infection.
- Onset: Develops quickly, usually over a day or two.
Chalazion:
- Pain: Generally painless, though it may feel heavy.
- Appearance: A firm, slow-growing lump, usually further back on the eyelid than a stye.
- Cause: A chronic blockage of an oil gland (not necessarily an active infection).
- Onset: Develops slowly over several weeks.
If you have a lump that is not painful but refuses to go away after several weeks, it is likely a chalazion rather than an active case of stye disease. However, an untreated stye can sometimes evolve into a chalazion if the inflammation becomes chronic.
When Should You See a Specialist?
Most styes are self-limiting and resolve within a week. However, certain “red flags” indicate that the infection has progressed beyond the point of stye disease home treatment. Consulting a specialist is necessary if you experience any of the following:
- Vision Changes: Can a stye cause blurred vision? Generally, a small stye will not affect your sight. However, if the swelling is severe enough to press against the eyeball or if the infection spreads to the cornea, it can definitely cause blurring or light sensitivity.
- Spreading Redness: If the redness and swelling extend beyond the eyelid to the cheek or other parts of the face, it may be a sign of cellulitis, a serious infection.
- Excessive Tearing or Discharge: Thick, yellow, or green discharge that makes it difficult to open your eyes in the morning.
- No Improvement: If the stye does not begin to drain or shrink after 48 hours of consistent home care.
Modern Treatment Options: From Eye Drops to Minor Surgery
In 2026, the treatment for stye disease has become highly efficient, focusing on clearing the infection while minimizing discomfort.
Medical Therapies
For many, a combination of topical treatments is sufficient. This may include antibiotic eye drops or ointments to target the Staphylococcus bacteria. If there is significant eyelid swelling and redness, a doctor might prescribe a mild steroid drop to reduce the inflammatory response. In cases of internal styes that are particularly stubborn, oral antibiotics may be necessary to reach the deep-seated infection.
Minor Surgical Intervention
If a stye does not respond to medication or turns into a persistent chalazion, a minor procedure called “Incision and Curettage” may be performed. Under local anesthesia, a specialist makes a tiny incision on the inside of the lid to drain the blocked gland. This procedure is quick, typically takes less than 15 minutes, and leaves no visible scarring.
Managing Systemic Links
For patients where autoimmune disease and styes go hand-in-hand, or those with graves eye disease stye issues, the treatment must address the underlying condition. Managing systemic inflammation is often the only way to break the cycle of recurring eyelid infections.
How to Prevent Recurrent Styes: 5 Golden Rules
Prevention is the cornerstone of ocular health. If you are prone to styes, incorporating these five rules into your daily routine can make a significant difference.
1. Practice Strict Hand Hygiene
Most bacterial eye infections start with your fingers. Avoid touching or rubbing your eyes throughout the day. If you wear contact lenses, ensure your hands are washed with soap and dried with a lint-free towel before handling your lenses.
2. Implement an Eyelid Scrub Routine
For those with dry eye disease and styes, keeping the eyelid margins clean is vital. Use a dedicated eyelid cleanser or diluted baby shampoo on a warm washcloth to gently scrub the base of your eyelashes every night. This removes the “biofilm” where bacteria love to hide.
3. Respect the “Period After Opening” (PAO)
Eye makeup is a breeding ground for bacteria. Never share cosmetics and replace your mascara and eyeliner every three months. If you develop a stye, discard all eye makeup you were using at the time to prevent re-infection.
4. The Power of the Warm Compress
Regularly applying a warm compress for 5–10 minutes can keep the oils in your Meibomian glands flowing freely. This is the best stye disease home treatment for both prevention and early-stage care, as it prevents the blockages that lead to internal styes.
5. Manage Underlying Conditions
If you have been diagnosed with blepharitis or rosacea, follow your specialist’s treatment plan strictly. Managing these chronic inflammatory conditions is the only way to prevent stye eye disease from becoming a recurring part of your life.
FAQ
How long does a stye usually last?
Most styes follow a predictable cycle of 7 to 10 days. They typically grow for 2–3 days, “point” or develop a head, drain naturally, and then heal over the remaining few days.
Is a stye contagious?
While the bacteria that cause a stye can be transferred, the stye itself is not “contagious” in the way a cold or the flu is. However, you should not share towels, pillowcases, or makeup with others while you have an active infection to avoid spreading the bacteria.
Can stress cause a stye?
Yes, indirectly. Stress weakens the immune system, making it harder for your body to fight off the Staphylococcus bacteria. Additionally, people under stress often sleep less and rub their eyes more frequently, both of which are risk factors.
How do I get rid of a stye overnight?
It is virtually impossible to resolve a bacterial infection overnight. Beware of “miracle” cures. The fastest way to heal is consistent warm compresses and avoiding the urge to “pop” the stye, which only spreads the infection deeper into the tissue.
Are styes contagious to other people?
Technically, the bacteria are transmissible, but it is unlikely for someone else to develop a stye just by being near you. Standard hygiene, like not sharing face towels, is enough to protect those around you.



