Few anatomical variations capture public curiosity as effortlessly as eyes featuring entirely different colors. This striking biological presentation, scientifically referred to as heterochromia, affects a tiny percentage of the global population. While it is frequently celebrated in popular culture for its rare aesthetic quality, medical professionals analyze the condition through a different lens. For clinicians, a mismatch in pigmentation represents a fascinating expression of cellular genetics and chemical distribution within the ocular tissue.
It is essential to recognize how the body expresses these unusual physical variations. Understanding the mechanics behind a heterochromia eye layout allows us to distinguish between normal biological diversity and subtle changes that may point to broader systemic shifts. While a vast majority of multi-colored variations are entirely benign configurations present from infancy, a sudden shift in pigmentation during adulthood requires meticulous investigation. This guide breaks down how iris color functions, the distinct categories of pigmentation variance, and when a change in eye color warrants a specialist’s intervention.
Table of Contents
What is Heterochromia?

To understand why heterochromia in eyes occurs, we must examine the physiological structure of the iris—the muscular, colored ring that expands and contracts to regulate the amount of light entering the eye. The color of your iris is determined by the concentration and specific layout of a pigment called melanin. Melanin is synthesized by specialized cells known as melanocytes, which are located deep within the iris stroma layer.
Get Free Consultation
Have any questions? Leave your details and we'll get back to you shortly.
Your genetic blueprint dictates how these melanocytes operate. High concentrations of the pigment produce dark brown eyes, while lower concentrations create shades of hazel, green, or amber. When a minimal volume of melanin is present, light scatters across the fibrous stromal matrix, generating a blue appearance. A disruption in the normal melanin distribution in iris tissue results in iris heterochromia, leading to an imbalance in coloration.
In medical literature, clinicians classify the condition using two distinct phrases depending on the scope of the pigment imbalance:
- Heterochromia iridum: Describes a total color discrepancy where one eye presents a completely different shade than its partner.
- Heterochromia iridis: Describes a scenario where a single iris features multiple, distinctly separated color sections.
When patients ask, “What causes heterochromia in eyes?” the underlying mechanism almost always traces back to a localized alteration in melanocyte activity during early cellular development, preventing even pigmentation.
The Three Primary Types of Heterochromia
This ocular variation does not manifest uniformly in every individual. Depending on the precise boundaries and concentration shifts of melanin across the stroma, medical science groups the trait into three major types of heterochromia.
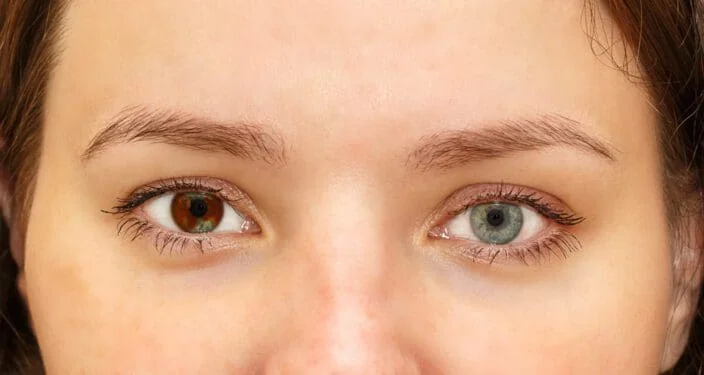
Complete Heterochromia
This is the most visually striking form of the trait, where one eye is a totally separate color from the other. An individual might have one rich brown eye and one light blue or green eye. This distinct mismatch is typically congenital, meaning the person was born with it. For the vast majority of individuals, this absolute difference exists as an isolated physical trait that carries no negative impact on visual acuity or general physical health.
Sectoral (Partial) Heterochromia
Often called partial heterochromia, sectoral heterochromia occurs when a distinct section or “slice” of a different color appears within the same iris. For example, a person may have a predominantly green eye, but a sharp, well-defined wedge of dark brown cuts across a portion of the iris, extending outward from the pupil. This partial expression can develop in one eye or both simultaneously, presenting a wide range of shapes and color pairings.
Central Heterochromia
This variation features a multi-toned appearance where an inner ring of one color encircles the pupil, while the outer portion of the iris exhibits a completely different shade. A classic example is a sharp golden or hazel ring surrounding the center, bordered by a field of clear blue or green on the outer margin. This presentation is often recorded under the technical term central heterochromia iridis.
Many people spend years wondering about the difference between hazel eyes and central heterochromia. Hazel eyes feature a diffuse, gradual blending of green, brown, and gold shades that bleed into one another across the entire surface of the iris.
Conversely, central heterochromia eyes show strict, sharp borders dividing the inner ring from the outer color field without any natural blending. When considering how common is central heterochromia, it is recognized as the most frequent form of pigment variance, though many mild expressions are misdiagnosed as hazel.
Congenital vs. Acquired Heterochromia: Root Causes
When checking the origin of a heterochromia in eyes layout, the primary medical objective is to identify the exact time of onset. The causes are divided into congenital forms (present from birth or early infancy) and acquired forms (developing during childhood or adulthood).
Congenital Variations
Most cases of multi-colored eyes are congenital and result from an isolated, harmless genetic mutation. This localized shift simply changes how melanin develops during embryonic growth. However, a small percentage of congenital cases may point to an underlying systemic condition:
- Waardenburg Syndrome: A rare genetic condition that can alter hair, skin, and eye pigmentation, occasionally presenting alongside congenital hearing differences.
- Congenital Horner Syndrome: Caused by a disruption in the sympathetic nerve pathways leading to one side of the face during development. The lack of nerve stimulation prevents melanocytes from darkening the iris fully, leaving the affected eye lighter.
- Sturge-Weber Syndrome: A congenital disorder characterized by unusual blood vessel configurations affecting the skin, brain, and ocular systems.
Acquired Variations
If a person notices a change in iris color later in life, the presentation is classified as acquired. Unlike congenital traits, an acquired shift can be a secondary symptom of an active localized issue or an external event.
Blunt force injuries, penetrating wounds or surgical complications can cause internal bleeding (hyphema), leaving iron deposits that permanently darken the iris tissue.
Other prominent causes of acquired shifts include:
- Fuchs Heterochromic Iridocyclitis: A chronic, low-grade form of internal eye inflammation (uveitis) that leads to iris tissue degeneration, causing the affected eye to appear noticeably lighter over time.
- Glaucoma Medications: Topical drop treatments designed to reduce intraocular pressure can trigger melanin production, causing a lighter iris to turn a darker brown shade.
- Intraocular Tumors: Benign growths or malignant melanomas developing inside the iris stroma can alter the visible color balance of the eye.
| Medical Classification | Onset Timeline | Common Underlying Causes | Clinical Urgency |
| Congenital | Birth or early childhood | Benign genetic variants, Waardenburg syndrome, Horner syndrome | Low (Monitored during standard pediatric check-ups) |
| Acquired | Adulthood or later childhood | Eye trauma, chronic internal inflammation, iris tumors, glaucoma drops | High (Demands immediate ophthalmic evaluation) |
When to See a Specialist: Identifying the Red Flags
If you have lived with mismatched eyes since your youth without changes in your sight, there is typically no reason for medical concern. However, learning when to worry about heterochromia relies on keeping a close watch on the stability of your iris pigmentation. Any new or evolving coloration requires an immediate evaluation.
You should contact an eye care professional without delay if you observe any of the following symptoms:
- A gradual or sudden change in the shade of one eye that was not present during your childhood.
- Persistent eye pain, a deep feeling of internal pressure, or chronic redness.
- New visual disturbances, such as unexpected blurring, light sensitivity, or flash/floater movements.
- A difference in the baseline size of your pupils or a drooping eyelid developing on one side.
An acquired shift is a signal that something has altered the cellular environment of your eye. Dismissing these red flags can allow chronic underlying issues, like uveitis or early-stage growths, to progress unnoticed, making timely diagnostics essential.
Diagnostics: What to Expect During an Ophthalmic Exam
When exploring why is my eye twitching or why an iris is changing color, an eye care specialist relies on sophisticated imaging tools to look beyond the surface. Diagnosing the root cause of an acquired change involves a detailed, comfortable clinical evaluation.
The cornerstone of this examination is a slit-lamp evaluation. This specialized binocular microscope focuses a high-intensity sheet of light into the anterior chamber of your eye. It allows the specialist to examine the structural health of your iris stroma, check for hidden signs of cellular inflammation, and scan for any abnormal tissue growths.
Additionally, the clinician will measure your intraocular pressure to rule out early-stage glaucoma. High-resolution digital photography may be utilized to capture a baseline image of your iris heterochromia, allowing the team to compare photos during future check-ups and ensure the pigment boundaries remain perfectly stable.
Managing Eye Health and Cosmetic Considerations
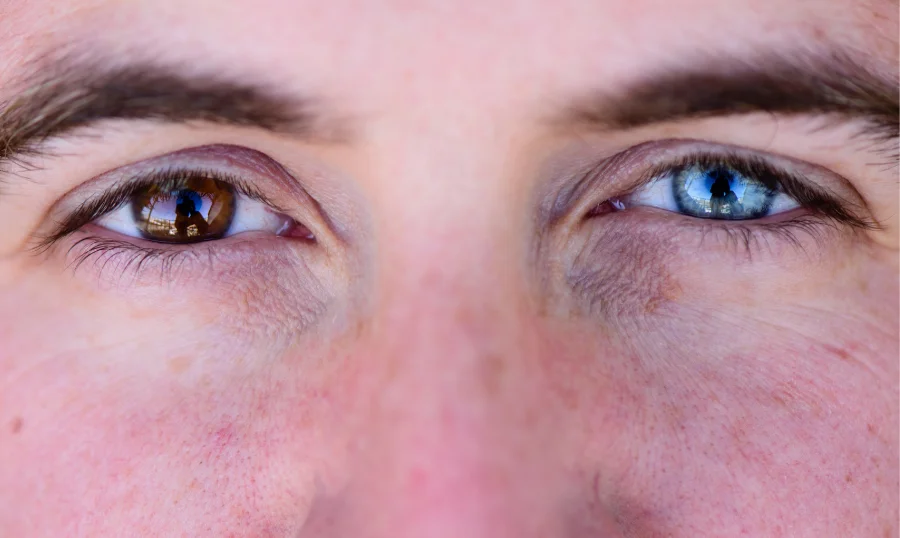
Because congenital variations are simply an alternative expression of melanin, they do not cause vision impairment and require no active medical treatment. The clinical focus for these natural presentations is centered around lifelong preservation.
UV Protection Strategies
Light-colored eyes naturally contain less protective melanin, making them more vulnerable to the damaging effects of ultraviolet (UV) radiation. If you have complete or sectoral heterochromia where one section of your iris is blue or light green, that specific area is more susceptible to UV strain. Wearing high-quality sunglasses that offer 100% protection against UVA and UVB rays is an essential habit for protecting the delicate internal structures of the eye from long-term solar damage.
Cosmetic Adjustments
While the vast majority of people embrace their multi-colored eyes as a unique and beautiful physical signature, some individuals may prefer a more uniform look. If an asymmetry causes self-consciousness, it can be managed by a professional fitting for opaque cosmetic contact lenses.
It is vital that any cosmetic lens is prescribed and monitored by a licensed optometrist. Using non-prescription fashion lenses purchased online or from unregulated sources can scratch the delicate corneal surface and introduce dangerous bacteria into the eye, risking permanent vision damage.
FAQ – Frequently Asked Questions
Is heterochromia a disease or a mutation?
On its own, congenital heterochromia is not a disease; it is a harmless genetic mutation. It is a biological variation that affects the concentration of melanin in the iris without altering the physical function of the eye or your ability to see clearly.
How rare is heterochromia in humans?
Complete heterochromia is exceptionally rare in humans, affecting fewer than 1% of the global population. When considering how rare is heterochromia, the congenital complete version is quite unusual, while subtle variations like central or sectoral patterns appear slightly more frequently.
Can you develop heterochromia later in life?
Yes, you can develop acquired heterochromia as an adult. If an eye color shift occurs later in life, it is typically an acquired condition triggered by factors such as a physical injury, chronic internal inflammation, or specific prescription eye drops.
Does heterochromia affect your vision?
No, the trait itself does not impact your visual acuity or your ability to process light and color. However, if your heterochromia is acquired, the underlying issue causing the color change can compromise your vision if left untreated.
When should you worry about heterochromia?
You should schedule a medical evaluation if your eye color changes suddenly or gradually during adulthood. If the color shift is accompanied by persistent pain, swelling, blurred vision, or changes in your pupil size, it requires urgent diagnostic attention.
Can eye color change naturally as an adult?
No, eye color does not change naturally or spontaneously as a healthy adult. While your eyes may appear to shift color due to changes in lighting, pupil size, or clothing reflections, the actual chemical pigmentation remains completely stable unless altered by an injury or an underlying medical condition.
Can stress or trauma cause a change in eye color?
Emotional or psychological stress cannot change your eye color. However, physical trauma to the eye can cause a permanent change. An injury can break small blood vessels inside the eye, leading to iron staining that darkens the iris, or it can cause tissue degeneration that leaves the iris looking lighter.



