Gastric Sleeve vs Gastric Bypass is one of the most frequently researched comparisons in bariatric surgery today. Individuals exploring long term weight loss solutions often encounter these two procedures as leading options. While both aim to support substantial weight reduction and metabolic improvement, their techniques, physiological impact, and long term considerations differ in meaningful ways.
Understanding Gastric Sleeve vs Gastric Bypass requires more than a surface level overview. It involves examining surgical mechanisms, expected outcomes, risk profiles, nutritional implications, and lifestyle adjustments. This guide provides a science based yet engaging analysis designed to answer the most relevant questions people ask when comparing these two procedures.
Table of Contents
What Is Gastric Sleeve vs Gastric Bypass and How Do They Work?
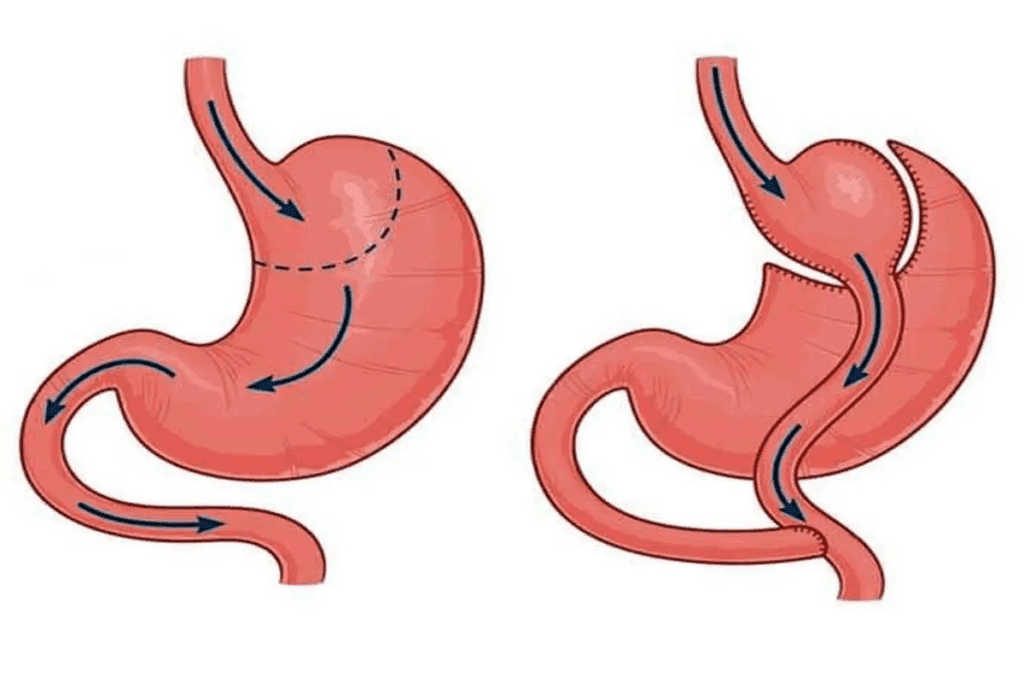
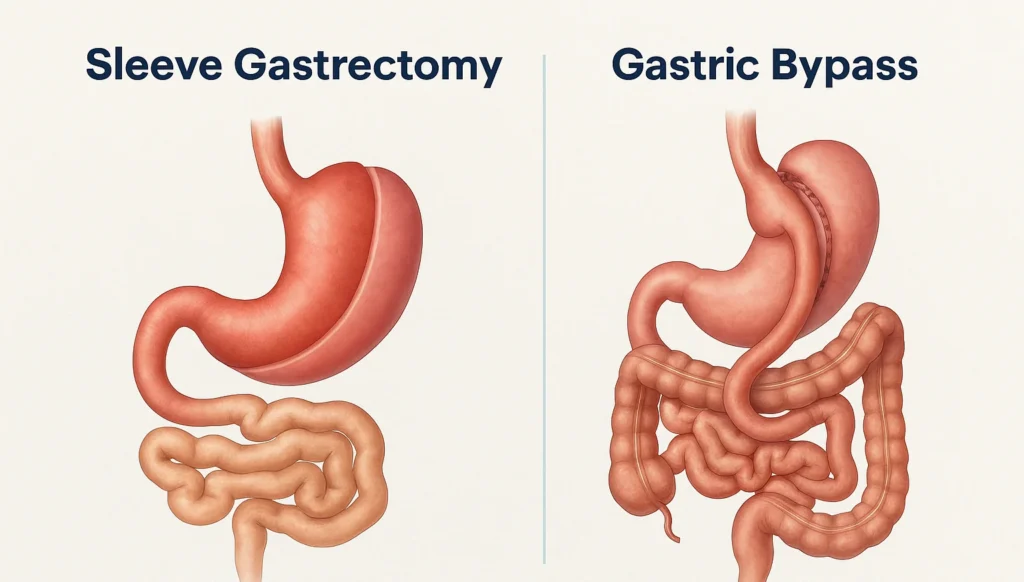
When discussing Gastric Sleeve vs Gastric Bypass, the first distinction lies in surgical design. Gastric sleeve surgery, also known as sleeve gastrectomy, involves removing a large portion of the stomach. The remaining stomach is shaped into a narrow tube. This reduces volume and influences hunger hormones such as ghrelin.
Get Free Consultation
Have any questions? Leave your details and we'll get back to you shortly.
Gastric bypass, medically referred to as Roux en Y gastric bypass, combines restriction with rerouting of the digestive tract. A small stomach pouch is created and directly connected to a segment of the small intestine. This bypasses part of the stomach and upper intestine, altering nutrient absorption and hormonal signaling.
In the context of Gastric Sleeve vs Gastric Bypass, the sleeve focuses primarily on restriction and hormonal modulation, while bypass introduces both restriction and malabsorption. This anatomical difference explains many of the contrasts seen in weight loss patterns, metabolic effects, and nutritional management.
Weight Loss Outcomes in Gastric Sleeve vs Gastric Bypass
Weight loss expectations are central to the Gastric Sleeve vs Gastric Bypass discussion. Clinical studies often show that both procedures can result in substantial excess weight loss within the first 12 to 24 months. However, trends indicate that gastric bypass may produce slightly greater average weight reduction over time.
Sleeve gastrectomy typically leads to progressive weight decline through portion control and reduced appetite. Bypass surgery often demonstrates faster early results due to both reduced intake and altered calorie absorption.
In comparative analyses of Gastric Sleeve vs Gastric Bypass, long term maintenance depends heavily on lifestyle adaptation, dietary habits, and metabolic response rather than the procedure alone. Individual variability plays a significant role, and published data emphasize trends rather than guarantees.
Comparative Overview
| Feature | Gastric Sleeve | Gastric Bypass |
| Surgical Type | Restrictive | Restrictive + Malabsorptive |
| Average Excess Weight Loss | High | Slightly Higher on Average |
| Hormonal Impact | Significant | Significant |
| Digestive Rerouting | No | Yes |
This table illustrates structural differences that influence outcomes in the Gastric Sleeve vs Gastric Bypass comparison.
Metabolic Effects and Diabetes Remission
Beyond weight reduction, metabolic improvement is a major consideration in Gastric Sleeve vs Gastric Bypass. Research suggests both procedures positively influence insulin sensitivity and blood glucose regulation.
Gastric bypass is often associated with rapid improvement in type 2 diabetes markers, sometimes occurring before significant weight loss. This phenomenon is linked to intestinal hormone changes and altered nutrient flow.
Sleeve gastrectomy also impacts metabolic hormones. Reduced ghrelin levels may decrease appetite and improve glucose regulation. In discussions of Gastric Sleeve vs Gastric Bypass, bypass is frequently noted for stronger early metabolic shifts, while sleeve demonstrates meaningful but sometimes more gradual changes.
Scientific literature highlights that remission rates vary based on duration of diabetes, pancreatic function, and patient characteristics. Therefore, metabolic outcomes in the Gastric Sleeve vs Gastric Bypass comparison are influenced by individual health history.
Risks and Complications in Gastric Sleeve vs Gastric Bypass
Every surgical procedure carries potential risks. In evaluating Gastric Sleeve vs Gastric Bypass, understanding complication profiles is essential.
Gastric sleeve surgery may involve risks such as leakage along the staple line, bleeding, or narrowing of the stomach tube. Because the intestinal pathway remains unchanged, nutritional deficiencies are generally less pronounced compared to bypass.
Gastric bypass introduces additional complexity due to intestinal rerouting. Potential concerns include internal hernias, dumping syndrome, and micronutrient deficiencies. For this reason, long term supplementation monitoring is emphasized in the Gastric Sleeve vs Gastric Bypass framework.
Importantly, advancements in minimally invasive techniques have reduced overall complication rates in modern bariatric surgery. Current data suggest both procedures have safety profiles comparable to other common abdominal surgeries when performed in experienced centers.
Nutritional Considerations and Lifestyle Adaptation
Nutritional management is one of the most discussed aspects of Gastric Sleeve vs Gastric Bypass. Since gastric bypass affects nutrient absorption, patients often require structured vitamin and mineral supplementation long term.
Sleeve patients also need nutritional awareness, though malabsorption is less significant. Protein intake, hydration, and balanced micronutrient consumption remain priorities in both procedures.
When examining Gastric Sleeve vs Gastric Bypass, lifestyle adaptation plays a defining role. Eating behaviors change dramatically after surgery. Smaller portions, mindful chewing, and structured meal timing become essential habits.
Key lifestyle adjustments typically include:
- Gradual transition from liquid to solid foods
- Emphasis on protein rich meals
- Reduced intake of refined sugars
- Routine medical follow up
In the broader conversation of Gastric Sleeve vs Gastric Bypass, long term success is strongly associated with behavioral consistency rather than the surgical technique alone.
Recovery and Long Term Maintenance
Recovery timelines are often similar in the Gastric Sleeve vs Gastric Bypass comparison. Most procedures are performed laparoscopically, which shortens hospital stays and accelerates return to daily activities.
However, gastric bypass may involve slightly longer operative time due to its complexity. Postoperative dietary stages are structured in both surgeries, progressing from liquids to pureed foods and eventually solid meals.
Long term maintenance in Gastric Sleeve vs Gastric Bypass depends on sustained follow up care. Clinical guidelines emphasize periodic blood tests, nutritional assessment, and monitoring of weight trajectory.
Studies tracking patients five to ten years after surgery suggest that both procedures can maintain meaningful weight reduction. Yet some data indicate a modest trend toward weight regain in certain sleeve patients, highlighting the importance of continued medical oversight.
Psychological and Quality of Life Dimensions
While the physiological aspects dominate most discussions, psychological adaptation is equally relevant in Gastric Sleeve vs Gastric Bypass. Research indicates that many patients report improved mobility, energy levels, and self perception after significant weight loss.
At the same time, surgery introduces emotional adjustments. Food often plays a social and psychological role, and post surgical dietary restrictions may require coping strategies.
In evaluating Gastric Sleeve vs Gastric Bypass, quality of life improvements are widely documented, but outcomes vary individually. Comprehensive bariatric programs frequently include nutritional counseling and behavioral support to address these changes.
Choosing Between Gastric Sleeve vs Gastric Bypass
Deciding between these procedures involves analyzing health history, body mass index, metabolic conditions, and personal preferences. The Gastric Sleeve vs Gastric Bypass decision is rarely one size fits all.
Factors often considered include:
- Presence of severe acid reflux
- History of abdominal surgery
- Degree of obesity
- Metabolic health status
- Willingness for long term supplementation
In many comparative evaluations of Gastric Sleeve vs Gastric Bypass, gastric bypass may be preferred for individuals with significant gastroesophageal reflux disease, while sleeve gastrectomy is often considered technically simpler.
Ultimately, the discussion surrounding Gastric Sleeve vs Gastric Bypass reflects a broader shift in obesity treatment. Bariatric surgery is increasingly recognized not only as a weight loss intervention but as metabolic therapy supported by decades of clinical research.
Understanding Gastric Sleeve vs Gastric Bypass in a Broader Context
The comparison of Gastric Sleeve vs Gastric Bypass highlights two scientifically established surgical strategies designed to support weight reduction and metabolic improvement. Both procedures demonstrate significant potential benefits, distinct mechanisms, and unique considerations.
Rather than framing the choice as a competition, the Gastric Sleeve vs Gastric Bypass discussion is best understood as a tailored medical decision shaped by physiology, research evidence, and individual health goals. Long term outcomes depend not only on anatomy but also on education, follow up care, and lifestyle commitment.
As scientific understanding evolves, the dialogue around Gastric Sleeve vs Gastric Bypass continues to expand, offering deeper insight into how surgical innovation intersects with metabolic science. For individuals exploring bariatric options, informed analysis remains the most powerful starting point.



