The term Dental Nerve often sparks anxiety, curiosity, and a surprising number of myths. In reality, the removal of a Dental Nerve is not about extracting a visible cord from the tooth but about treating infected or inflamed pulp tissue inside the root canal system. At WellDemir, we believe that understanding what happens during a Dental Nerve procedure reduces fear and replaces it with informed confidence.
Table of Contents

What Is the Dental Nerve and Why Does It Matter?
The Dental Nerve is not a single isolated thread. It is part of the dental pulp, a soft tissue complex located in the center of the tooth. This pulp contains nerve fibers, blood vessels, connective tissue, and specialized cells that help in tooth development. When people refer to the Dental Nerve, they usually mean this inner pulp tissue.
In a healthy tooth, the Dental Nerve plays a sensory role. It responds to temperature, pressure, and trauma. However, once the tooth has fully developed, its survival does not depend on the pulp. That means a tooth can function normally even after the Dental Nerve is removed, provided the surrounding structures remain intact.
Get Free Consultation
Have any questions? Leave your details and we'll get back to you shortly.
Inflammation of the Dental Nerve can occur due to deep decay, trauma, repeated dental procedures, or cracks. When bacteria invade the pulp chamber, the confined environment prevents swelling from expanding outward. Pressure builds up internally, often causing persistent pain.
When Does a Dental Nerve Need to Be Removed?
Removal of the Dental Nerve is typically associated with root canal therapy (endodontic treatment). The decision is not based on mild discomfort but on evidence of irreversible pulp inflammation or infection. Dentists assess symptoms, radiographic findings, and vitality tests before proceeding.
Common indicators include:
- Prolonged sensitivity to hot or cold
- Spontaneous throbbing pain
- Swelling near the tooth root
- Darkening of the tooth structure
- Radiographic signs of periapical infection
It is important to understand that not every toothache requires Dental Nerve removal. In some cases, the pulp can recover. In others, untreated infection may spread beyond the tooth apex into surrounding bone tissue.
Scientific literature suggests that bacterial biofilm plays a central role in pulp infection. Once bacteria colonize the pulp chamber, the immune response inside the confined tooth space can intensify tissue breakdown. At that stage, removing the Dental Nerve becomes a biological necessity rather than an elective choice.
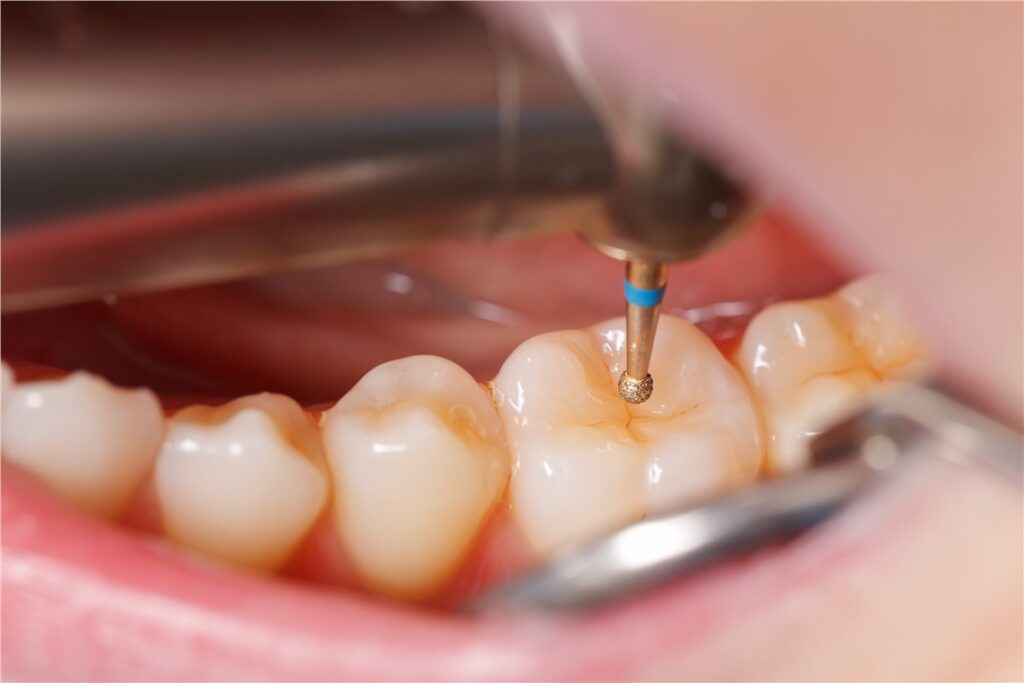
How Is the Dental Nerve Removed During Root Canal Treatment?
The removal of a Dental Nerve occurs during a structured endodontic procedure. The process involves precision rather than force. The dentist does not “pull out” a visible nerve but cleans and shapes the internal canal system.
The procedure generally follows these steps:
| Step | Procedure Phase | Purpose |
| 1 | Local anesthesia | Ensures patient comfort |
| 2 | Access cavity preparation | Reaches the pulp chamber |
| 3 | Pulp tissue removal | Eliminates infected Dental Nerve |
| 4 | Canal cleaning and shaping | Removes bacteria and debris |
| 5 | Irrigation and disinfection | Reduces microbial load |
| 6 | Filling and sealing | Prevents reinfection |
After anesthesia is applied, a small opening is made through the enamel and dentin. Specialized instruments called endodontic files are inserted into the canal system. These tools remove the inflamed or necrotic Dental Nerve tissue while shaping the canals for sealing.
Irrigation solutions are used to dissolve organic remnants and disinfect areas that mechanical instruments cannot reach. Finally, the cleaned canals are filled with a biocompatible material to seal the internal space.
Contrary to popular belief, modern Dental Nerve removal techniques are minimally invasive and guided by magnification, digital imaging, and advanced rotary systems.
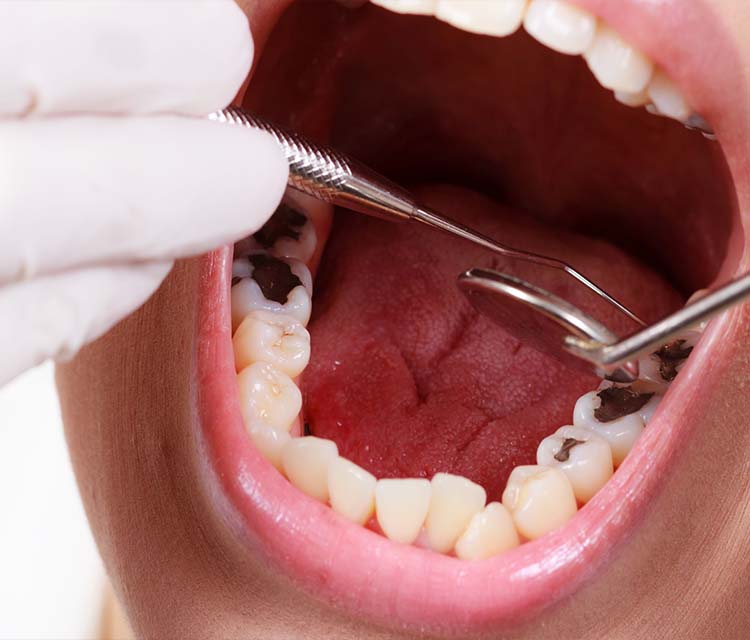
Does Removing the Dental Nerve Hurt?
One of the most persistent concerns is pain. Interestingly, the procedure to remove a Dental Nerve is typically less painful than the untreated infection itself.
Local anesthesia blocks nerve conduction before treatment begins. During the removal of the infected Dental Nerve, patients often report pressure sensations rather than sharp pain. Mild tenderness after the procedure may occur due to inflammation in surrounding tissues.
Research indicates that post treatment discomfort is often linked to pre existing inflammation rather than the removal of the Dental Nerve itself. Modern techniques aim to reduce apical extrusion of debris, which historically contributed to postoperative sensitivity.
Understanding the biological cause of pain helps demystify the experience. The inflamed Dental Nerve generates intense signals due to internal pressure. Once removed, that internal source of pain is eliminated.
What Happens After the Dental Nerve Is Removed?
After the Dental Nerve is removed, the tooth loses its sensory function but retains structural capability. It no longer responds to temperature changes, yet it continues to function in chewing and biting.
Over time, a tooth without a Dental Nerve may become slightly more brittle. This is why dentists often recommend protective restorations such as crowns in structurally compromised cases. The decision depends on the amount of remaining tooth structure.
Biologically, surrounding periodontal tissues continue to supply nutrients through external blood vessels. The absence of the Dental Nerve does not mean the tooth is “dead” in the way many imagine. It simply means the internal pulp tissue has been replaced with a sealed, inert filling material.
In long term observations, properly treated teeth without a Dental Nerve can remain functional for decades, provided oral hygiene and restorative integrity are maintained.
Are There Alternatives to Dental Nerve Removal?
In some early cases of pulp inflammation, conservative approaches may allow the Dental Nerve to recover. Vital pulp therapy, indirect pulp capping, or partial pulpotomy may preserve part of the pulp tissue.
However, once irreversible pulpitis or necrosis occurs, complete removal of the Dental Nerve becomes the predictable solution. Delaying treatment in such cases may increase bacterial spread beyond the root tip.
Emerging regenerative endodontics explores the possibility of restoring damaged pulp tissue, particularly in immature teeth. Research in tissue engineering suggests that scaffolds, stem cells, and growth factors may one day reduce the need for traditional Dental Nerve removal in specific cases.
While these developments are promising, conventional root canal therapy (endodontic treatment) remains the most established method for managing infected pulp tissue.
Scientific Perspective on Dental Nerve Removal Success Rates
Clinical studies often report high success rates for procedures involving Dental Nerve removal when performed under proper protocols. Success depends on thorough cleaning, effective sealing, and coronal restoration quality.
Factors influencing long term outcomes include:
- Initial extent of infection
- Canal anatomy complexity
- Quality of disinfection
- Integrity of final restoration
- Patient oral hygiene habits
Advanced imaging methods, such as cone beam computed tomography, allow more accurate visualization of root canal morphology. This improves the predictability of Dental Nerve removal procedures.
At WellDemir, diagnostic precision and procedural accuracy are emphasized to ensure that each Dental Nerve treatment aligns with current scientific standards.
Understanding the Dental Nerve Removal Process
The removal of a Dental Nerve is not a dramatic extraction of a visible structure but a controlled biological intervention inside the tooth. It is performed when infection or irreversible inflammation compromises pulp health. Through careful cleaning, disinfection, and sealing, the internal canal system is restored to a stable state.
By understanding how the Dental Nerve functions and why it may need removal, patients can approach treatment with clarity rather than fear. The goal is not simply to eliminate pain but to preserve the natural tooth structure whenever possible.
At WellDemir, transparency, evidence based methodology, and patient education remain central to every procedure involving Dental Nerve care.



I had a similar treatment done in Istanbul and can confirm the quality is world-class. Highly recommend Turkey for dental care.
We’re delighted you found this helpful! Don’t hesitate to contact us if you have further questions. Our team is always happy to help.
Really well written and informative. The cost comparison with UK prices is particularly eye-opening for dental work.
Very informative article! I’ve been considering dental treatment in Turkey and this helped me understand the process much better. Thank you for the detailed explanation.