Bariatric surgery has evolved significantly over the last few decades, yet no procedure guarantees lifelong success for every patient. In cases where weight loss surgery (bariatric metabolic surgery (diabetes remission surgery)) fails or complications arise, surgeons frequently explore revision options. Among these solutions, Duodenal Switch has gained attention as a powerful revisional strategy. The procedure combines restrictive and metabolic mechanisms, which is one reason many specialists consider Duodenal Switch when earlier bariatric surgeries do not produce the desired outcomes.
For patients who have undergone procedures such as gastric sleeve (laparoscopic sleeve gastrectomy) or gastric bypass (Roux-en-Y gastric bypass) and later experience weight regain, unresolved metabolic issues, or surgical complications, revisional surgery may become part of the discussion. In these situations, Duodenal Switch is sometimes evaluated because of its unique physiological approach.
Table of Contents

Understanding the Concept Behind Duodenal Switch
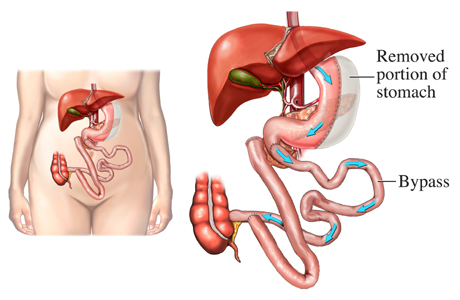
The procedure known as Duodenal Switch is a complex metabolic surgery (diabetes remission surgery) that modifies both stomach size and nutrient absorption pathways. Unlike purely restrictive procedures, Duodenal Switch combines sleeve gastrectomy with intestinal rerouting, which changes how the body processes calories and nutrients.
Get Free Consultation
Have any questions? Leave your details and we'll get back to you shortly.
In simple terms, the stomach is reduced in size while the digestive tract is rearranged so that food travels through a shorter portion of the small intestine. This alteration may affect how calories and fats are absorbed. Because of this dual mechanism, Duodenal Switch is often associated with significant metabolic effects compared to many other bariatric procedures.
Another characteristic of Duodenal Switch is the preservation of the pyloric valve, the muscular valve that regulates food flow from the stomach to the small intestine. Some surgeons believe this anatomical preservation may help reduce certain complications seen in other surgeries, such as dumping syndrome. These anatomical differences are one reason why Duodenal Switch remains a topic of discussion in revisional bariatric surgery.
Why Duodenal Switch Is Considered in Bariatric Revision Cases
When a previous weight loss surgery (bariatric metabolic surgery (diabetes remission surgery)) fails to achieve long term goals, physicians may explore different revisional approaches. One frequently discussed option is Duodenal Switch, especially when metabolic improvement is a priority.
Several factors may lead surgeons to consider Duodenal Switch in revision scenarios:
- Previous restrictive procedures may lose effectiveness over time
- Hormonal changes may not have been sufficient after the first surgery
- Significant weight regain may occur years after the initial procedure
- Some metabolic conditions remain unresolved
Because Duodenal Switch influences both restriction and absorption, it provides a broader metabolic intervention compared to surgeries that focus only on stomach size. For this reason, some specialists view Duodenal Switch as a potential solution when earlier procedures fail to deliver lasting metabolic results.
Another reason surgeons may evaluate Duodenal Switch is the procedure’s potential impact on hormonal signals related to appetite, satiety, and insulin regulation. These metabolic effects can play an important role in long term weight management discussions.
How Duodenal Switch Differs From Other Revisional Procedures
Many bariatric revision procedures involve converting one surgery into another. For example, sleeve gastrectomy may be converted into gastric bypass (Roux-en-Y gastric bypass), or gastric banding may be revised into sleeve surgery. However, Duodenal Switch introduces a more comprehensive anatomical and metabolic change.
Below is a simplified comparison of several revision options.
| Revision Procedure | Main Mechanism | Metabolic Impact | Structural Change |
| Gastric Bypass Revision | Restriction + mild malabsorption | Moderate | Moderate |
| Sleeve Revision | Restriction | Limited | Mild |
| Duodenal Switch | Restriction + strong malabsorption | Significant | Extensive |
Because Duodenal Switch modifies both the stomach and intestinal pathway, it often creates a more pronounced metabolic shift compared to some alternatives. This characteristic is why many surgeons examine Duodenal Switch when addressing severe weight regain or metabolic relapse.
It is important to note that the complexity of Duodenal Switch also requires extensive surgical expertise and careful patient evaluation. Not every patient who had a previous bariatric procedure is automatically considered a candidate for Duodenal Switch.
Metabolic Effects Associated With Duodenal Switch
One of the most frequently discussed aspects of Duodenal Switch is its metabolic influence. While weight reduction is often part of the conversation, metabolic regulation plays an equally important role in why surgeons analyze Duodenal Switch as a revisional option.
The surgery alters the digestive pathway so that food mixes with digestive enzymes later in the intestinal process. This mechanism may affect how the body absorbs fats and calories. Researchers studying Duodenal Switch often examine how these changes influence insulin sensitivity, hormone production, and gut microbiota.
Several hormones associated with appetite and metabolism may shift following Duodenal Switch, including:
- GLP-1
- Ghrelin
- Peptide YY
These hormonal changes may contribute to appetite regulation and satiety signals. Because revisional patients sometimes struggle with persistent metabolic conditions, Duodenal Switch is frequently discussed in metabolic surgery (diabetes remission surgery) research as a powerful intervention.
However, the metabolic complexity of Duodenal Switch also requires long term nutritional monitoring, which is why surgeons often emphasize comprehensive follow up when discussing Duodenal Switch as a revision procedure.
Surgical Challenges and Considerations With Duodenal Switch
Although Duodenal Switch offers unique metabolic characteristics, it is also considered one of the more technically demanding bariatric procedures. Revision surgery itself introduces additional complexity, and converting previous operations into Duodenal Switch may require careful surgical planning.
Some considerations surgeons evaluate before recommending Duodenal Switch include:
- Type of previous bariatric surgery
- Scar tissue from earlier operations
- Current metabolic conditions
- Nutritional status of the patient
- Anatomical changes caused by the first procedure
Because of these variables, the decision to perform Duodenal Switch is rarely made quickly. Instead, surgeons typically conduct detailed imaging, laboratory testing, and multidisciplinary assessments before considering Duodenal Switch as a revision option.
The technical nature of Duodenal Switch also means that surgical teams performing the procedure usually specialize in advanced bariatric and metabolic surgery (diabetes remission surgery).
Long Term Research and Outcomes Linked to Duodenal Switch
Scientific discussions around Duodenal Switch often focus on long term outcomes. Studies examining bariatric procedures over extended periods frequently compare metabolic effects, weight trends, and complication profiles.
In several research analyses, Duodenal Switch has demonstrated strong metabolic results in carefully selected patients. Because the procedure alters nutrient absorption pathways, long term weight regulation and metabolic improvement are often key areas of interest when evaluating Duodenal Switch.
However, these outcomes also depend on patient adherence to follow up care. Nutritional supplementation, dietary monitoring, and regular medical assessments are commonly associated with the postoperative management of Duodenal Switch.
Researchers continue to analyze how Duodenal Switch performs compared with other revision strategies. As bariatric science evolves, new surgical techniques and variations of Duodenal Switch continue to emerge, expanding the conversation around metabolic surgery (diabetes remission surgery).
The Role of Duodenal Switch in Modern Bariatric Strategy
The landscape of bariatric surgery is constantly evolving. Procedures once considered experimental have become standard, while others have been refined through decades of surgical experience. Within this evolving field, Duodenal Switch remains one of the most complex and metabolically impactful procedures available.
For patients who previously underwent bariatric surgery and later experienced limited success, surgeons sometimes evaluate Duodenal Switch as a possible revisional approach. Its ability to combine stomach reduction with intestinal modification distinguishes it from many other surgical options.
Despite its potential benefits, Duodenal Switch is not universally recommended. Each case is typically evaluated individually, taking into account surgical history, metabolic goals, and long term follow up requirements.
What remains clear is that Duodenal Switch occupies a unique position in bariatric surgery discussions. As research continues and surgical techniques improve, the procedure will likely remain an important topic in the field of metabolic and revisional bariatric surgery.
Revisional bariatric surgery represents one of the most complex areas of metabolic medicine. When earlier procedures fail to produce lasting outcomes, surgeons may explore a range of options, including Duodenal Switch. Because it combines restrictive and malabsorptive mechanisms, Duodenal Switch offers a distinctive physiological approach compared with many other bariatric procedures.
Its metabolic influence, hormonal effects, and anatomical design contribute to why some specialists examine Duodenal Switch during revision planning. At the same time, the complexity of Duodenal Switch requires experienced surgical teams and careful patient evaluation.
As bariatric research continues to expand, the role of Duodenal Switch in revisional surgery will likely remain a subject of ongoing study, clinical debate, and medical innovation.



Very informative article! I’ve been considering bariatric surgery in Turkey and this helped me understand the process much better.
We appreciate your feedback! Our medical team would be happy to answer any additional questions during a complimentary consultation.
The information about pre-surgery preparation is something I haven’t seen covered this well anywhere else.